Proton Therapy
What comes along to the patient?
Further information concerning:
Clinical stay at the Charité eye infirmary
In the course of the consultation hours, the ophthalmologist makes a choice for the best therapy option and decides whether further hospital treatment is needed. After confirmation of the tumour diagnosis, its location and dimensions have to be determined.
For this purpose, small tantalum marker clips are sutured to the sclera of the patient's eye by a surgeon. He then measures shape and location of the tumour in relation to the marker clips. These clips will in general cause no trouble to the patient and will therefore not been removed after proton therapy.
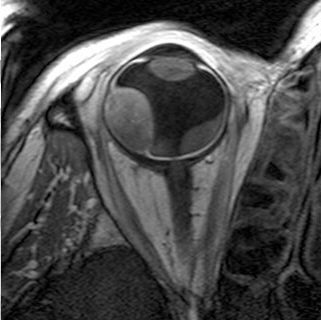
The performance of irradiation of the human eye requires a high-precision patient alignment and exact data of the inner eye structure. For this, several imaging techniques like computed tomography and magnetic resonance imaging are provided. Tomography serves mainly for a save and careful treatment planning, whereas the marker clips guarantee a reliable and precise patient positioning according to the individual treatment plan.
Preparation for the precision patient positioning
Short time after the surgical clip insertion, the patient will get his first appointment with our specialists for proton therapy at the HZB. During a simulation session, they individually manufacture a mask and a bite block to fasten the patient's head. The mask allows the immobilisation of the patient while he is sitting on the treatment chair that can be moved with a reproducibility of one tenth of a millimetre along three linear and two rotational axes.
For a series of fixation angles, X-ray pictures are taken with the chair locked in treatment position. We measure the eye position and orientation to determine the marker clip coordinates and to reconstruct the eye within the coordinate frame of the irradiation unit.
Together with the clinical data, the collected positioning data are used to construct a three-dimensional model of the eye and its inner structure within our image-based treatment planning system. With this model, our medical physicists are able to reconstruct exactly the target volume connected with the tumour and to calculate an optimum treatment position and fixation angle of the eye.
The medical physicists periodically discuss their treatment plans together with ophthalmologists and radiation oncologists before completion. As soon as the treatment plan has met the physicians' approval, the patient will get a feasibility check. For this, the treatment chair is locked in the final position that is intended for therapy. The patient has to look at the calculated position of a special fixation light. Once more, X-ray pictures are taken and the position both of the treatment chair and the fixation light are corrected as long as all detected marker clips are in perfect agreement with their calculated reference positions from the treatment plan. Then, proton beams are simulated with a light field. Our radiation therapists use eye lid retractors to drag the lids out of the field. If necessary, the treatment plan can be modified during simulation. When the simulation of the irradiation has succeeded, all chair coordinates are saved and the patient collimator is manufactured in the mechanical workshop.
Since the positioning procedure is always the same, the patient this way becomes acquainted with the similar treatment procedure that will take place later on.
Radiotherapy with protons
The irradiation is performed during the radiotherapy week on four consecutive days. The coordinates of the treatment chair and the fixation light are set to the previously stored positions and, this way, the patient is installed in the treatment position. Positioning is checked with X-ray pictures again. The position of the tumour eye is monitored by a TV camera and is to be marked on the TV screen. During irradiation, a possible movement of the eye will immediately be detected and the beam will be interrupted. As soon as the patient has reached his final treatment position again, the therapist will continue proton therapy simply at the touch of a button. Typical irradiation times for the dose application are about 30 seconds to 1 minute for each day, whereas the patient preparation and positioning takes about 15 minutes to half an hour of time.
Before the start and after completion of the irradiation, the radiation oncologist will explain the treatment plan, talk about the expected therapy success, and give recommendations according the follow-up procedure. Several months later in Berlin, the ophtalmologist will review the tumour damage and will observe its future degradation.